Participate in Health Canada’s consultation on access to ingredient information for food products sold online and take part in our townhall. Find out the latest on the specialty infant formula shortage and get access to a new resource from Health Canada. Learn what’s new in food allergy research, including a study on the role of probiotics in oral immunotherapy in children, and another study on grass pollen being a co-factor influencing the potential severity of an allergic reaction. Plus, check out this month’s mythbuster on whether epinephrine is dangerous.
Advocacy in action: Access label. Add to cart. Participate in Health Canada’s consultation on accurate ingredient information for online foods by July 8th
Health Canada is proposing new guidance for food products being sold online in Canada.
Your voice is needed to help ensure these changes happen.
When you buy food online (e.g., groceries, take-out, delivery), you may not be given the same level of ingredient information as you would see on the label of products you purchase in person. This lack of transparency can lead to purchasing products or ordering food that may not be safe options for you or your family, and it may prevent you from purchasing any food products online.
Health Canada is proposing new guidance to specifically address the need for clear labelling of food allergens.
Learn more and participate in the consultation at foodallergycanada.ca/AccessLabel by July 8, 2022.
Plus, find out more actions you can take, including participating in our townhall on June 15th, and taking our short survey by June 17th.
Advocacy in action: Specialty infant formula shortage – new resource from Health Canada

Last month, Health Canada issued a public advisory about the current shortage of specialty formulas for babies with food allergy. This shortage has resulted from the closure of a large manufacturing plant in the United States which is affecting the global availability of infant formula.
There is no current shortage of regular infant formula.
We are in ongoing conversations with healthcare providers, Health Canada and industry to help provide support to infants impacted by the shortage. If you are impacted, we strongly recommend you seek the guidance of your healthcare provider on options that may be available to you.
New resource from Health Canada
Health Canada has released information to help guide impacted families which specifies the types/brands of infant formula affected by the shortage, possible alternative approaches and products, and more.
Some of their tips on what to do during the shortage include:
- Breastfeeding your baby, if you can
- Maintaining or increasing your breastmilk supply if you are combining bottle-feeding and breastfeeding
- Trying a different brand of formula under the recommendation of your healthcare provider
- Introducing solid foods when your baby is about 6 months old
Download their resource for more information.
During this shortage, we’re working hard on your behalf to ensure your needs are being addressed. We will continue to keep you updated as the situation evolves.
As we learn more, if you want to hear directly on this topic, please email us at info@foodallergycanada.ca to let us know.
Research: What is known about the role of probiotics in OIT?

The role of probiotics in oral immunotherapy (OIT) is reviewed in a recent study. Find out more about this study in the following article provided by Atai Ariaz, Jessica Schneider, Hannah Silverman, and Joshua F.E. Koenig, Ph.D. – Researchers at the Schroeder Allergy and Immunology Research Institute at McMaster University.
Although there is currently no cure for food allergy, OIT is capable of raising the threshold of an allergen that a food allergic person can tolerate without triggering an allergic reaction. Individuals who are protected from reactions after stopping OIT are said to achieve “remission,” although most people relapse into allergy within one year.
Researchers are investigating ways to maximize the benefits of OIT by adding interventions such as drugs and probiotics as part of the treatment. A new study by Dr. Mimi Tang’s team in Australia investigates how the combination of OIT plus probiotics impacts the body’s immune response.
The key findings of this research
Dr. Tang’s team investigated the impact of treatment with peanut OIT plus probiotics on the genes expressed by certain immune cells. One of the important players in food allergy and the allergic response are immune cells called “Th2 cells.” The researchers investigated whether genes associated with Th2 cells are changed by the combination treatment of OIT and probiotics. They compared immune cells from children with peanut allergy who received OIT plus probiotics with cells from children who received a placebo. They found that immune cells from children who received placebo had a high expression of Th2 genes. In contrast, cells from children who underwent OIT plus probiotics had an altered gene profile with fewer characteristics of allergy-inducing Th2 cells. Since the experiment did not include a group that received immunotherapy without probiotics, it cannot be determined if the effect is due to the probiotics.
The researchers found that with OIT plus probiotics there was a remission at 3-months following treatment. It’s not known whether these changes can continue to protect patients beyond 3 months after therapy is stopped.
Possibilities for informing food allergy therapies of the future
Future allergy therapies can build on this research to identify potential genes and pathways that can be targeted in immune cells to maximize the benefit of OIT.
Do probiotics have a role in OIT?
If the question is whether you or your children should pursue OIT plus probiotics, it is important to note that this and other studies have not demonstrated that adding probiotics provides additional benefits compared to OIT alone. It is something that can be discussed with your allergist. We and other research groups are continuing to explore novel therapies to accompany OIT, hopefully making it safer and better in the long term.
Thank you for your insights Atai, Jessica, Hannah, and Joshua on this topic! Learn more about OIT.
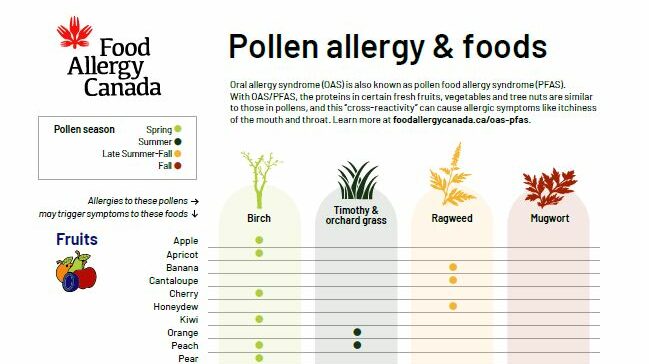
Research: Grass pollen as a co-factor in kids with food allergy, asthma
Co-factors, like uncontrolled asthma, influence the potential severity of an allergic reaction as they can lower the threshold at which one reacts. It’s important to understand your own personal co-factors so you can manage them and keep them under control.
A recent study discusses grass pollen as a potential co-factor in kids with food allergy, asthma, hay fever, or eczema.
Learn more
 Study: Children With Food Allergy Are at Risk of Lower Lung Function on High-Pollen Days
Study: Children With Food Allergy Are at Risk of Lower Lung Function on High-Pollen DaysResearch: U.S. approves first treatment option for EoE patients
The U.S. Food and Drug Administration (FDA) has approved Dupixent® (dupilumab) for patients aged 12 and older with eosinophilic esophagitis (EoE). With its approval, Dupixent is the first medicine available in the U.S. indicated to treat EoE in these patients.
This announcement provides hope for EoE treatment options; we will continue to share news about EoE therapies with you. Currently in Canada, Jorveza™ is the only medication approved by Health Canada to treat EoE in adults.
For more details, read the press release.
Learn more about EoE in our new section at foodallergycanada.ca/eoe.
Mythbuster: Is epinephrine dangerous?

FACT: Epinephrine is safe to use. It is the drug form of the hormone adrenaline that your body makes on its own. When an epinephrine auto-injector is given to treat anaphylaxis, it opens up the airways so it’s easier to breathe and improves blood pressure – it helps stops the reaction from progressing. After treating the allergic reaction, it’s recommended that you go to the hospital for further treatment and/or evaluation. Keep in mind that the reaction is the reason for going to the hospital, not because epinephrine has been used.
Learn more
 Facebook Live for families: Using epinephrine auto-injectors for treating anaphylaxis and teaching children how to use them
Facebook Live for families: Using epinephrine auto-injectors for treating anaphylaxis and teaching children how to use them